
The application of social innovation in healthcare: a scoping review | Infectious Diseases of Poverty
Overview of studies included
A total of 27 studies met the eligibility criteria and were included in the scoping review (Fig. 3). The majority of articles (21/27) were published between 2015 and 2020. Half (14/27) were published in health-specific journals and the remaining half in a range of other disciplines including management and business studies and programme, policy and planning studies, innovation and informatics, and agriculture. The most common methods were case studies (14/27), and scoping, systematic and general literature reviews (4/27). The literature was dominated by research originating from high-income country contexts, particularly in Europe. Nine published studies were conducted in low-income, low-middle income or upper-middle countries (two in Africa; four in Asia; three in Latin America). Low-income country researchers (first author) and institutions were under-represented in the sample, limited to only three representing institutions in Colombia, Uganda and India.
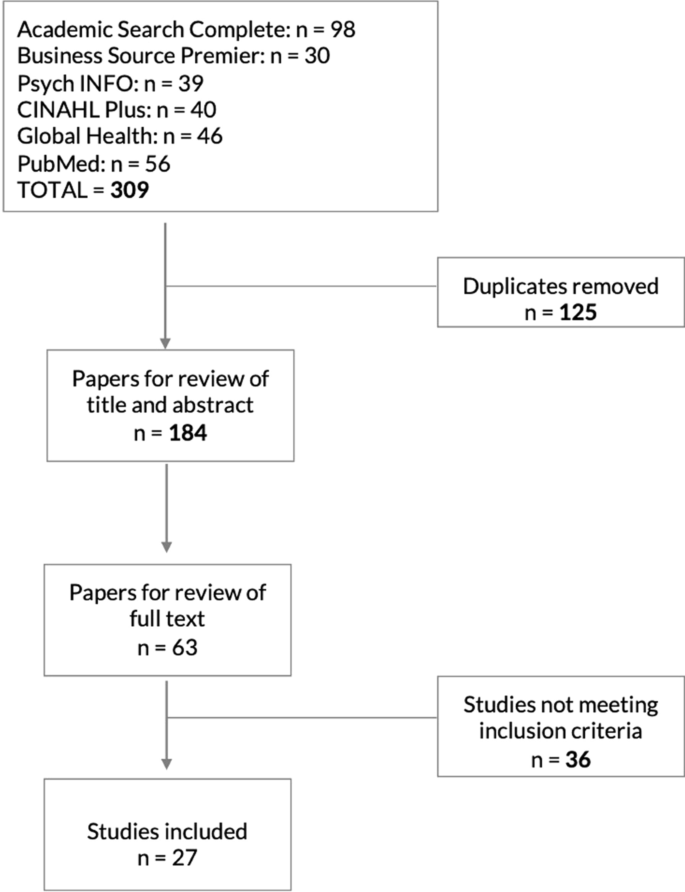
Literature search and review process
Focus
Social innovation has been applied to a variety of disease focus areas and to meet public health policy objectives (Table 2). Social innovations in low- and middle-income countries (LMICs), 3/27 studies, focused on infectious diseases, targeting prevention and access to services for malaria, HIV and Chagas disease [61,62,63,64]. A second focus of social innovations in LMICs, 9/27 studies, was to achieve equity in access to care and this included women’s health issues and social determinants of health such as poverty, rurality, and infrastructure (basic sanitation) [61, 64, 65]. These focus areas were in line with both national health agendas as well as global agendas as set by the Millennium and Sustainable Development Goals. The literature from high-income countries describes a different application of social innovation in terms of disease focus and public health objectives. Many European countries have adopted social innovation to address welfare state failures, particularly related to the inability of governments to sustain rising health expenditures for ageing populations [66,67,68,69,70,71,72]. In this context, social innovations have also been developed in response to policy objectives concerning public participation in health, often as a secondary strategy to move the burden of care from the state to individuals and other actors through social enterprise [71, 73,74,75]. As this indicates, social innovation is typically applied to address health system failures. Kreitzer et al. [76], for example, explored the Buurtzorg (Neighbourhood Care) Model in the Netherlands, designed to overcome vertical service delivery, low health worker satisfaction, and burdensome bureaucratic processes of care. De Freitas et al. [73] presents a participatory process involving families of patients affected by congenital disorders in the design interventions in areas where health systems responsiveness is poor, and Windrum et al. [77] presents the case of creating a standardised diabetes prevention and management programme based on patient-centred principles. This programme led to the reform of care provision across multiple countries.
Form and function
The classification of social innovations was problematic because of their divergent operational definitions. Two articles provided a proposed typology for social innovations in health. Mason et al. [66] proposed four types of social innovations in health equity: as social movements; services; social enterprises; and digital products. Farmer et al. [74] proposed a typology developed by frontline providers to promote child dental health as: extending existing practices; developing cheaper versions of existing products; adapting existing practices in different contexts or practice spaces; and translating ideas directly from evidence. From these cases studies of specific social innovations, however, the proposed typologies proved too narrow or restrictive as classification structures. The case studies fell into two functional categories, with social innovation treated either as a process or an outcome.
Four studies focused on social innovation as a process. These studies employed participatory mechanisms to support the development of new solutions to local challenges. The goal in all cases was to enhance patient or public participation in health care and enhance social relationships. Collaborative workshops occurred in the form of design sprints, co-design processes and think tank methodologies [73, 74, 81]. All these workshops were led by professional facilitators who were described as being ‘bricoleurs’, providing inspiration to participants, protecting the innovations, and linking them to resources. Srinivas [63], for example, presented a case that used crowdsourcing contests to give men who have sex with men the opportunity to design health promotional material to encourage other men to test for HIV.
Where social innovations were described as an outcome, models included different components (services, products, processes, social movements) and delivery in different settings. Neither single component of the model was particularly unique, but the combination or ‘bricolage’ of these components resulted in innovation. Three types of models were identified: care models (6/27 studies); social network/connection models (3/27 studies); and entrepreneurial models (2/27 studies) (Table 3). These models may or may not have a digital component or a financial component. Innovation in care models involved the re-organisation of care processes, including how services were delivered, often moving facility-based services directly into the community, with the role and scope of providers modified to give more autonomy or allow for task-shifting to non-health professionals [63, 70, 76, 77, 80, 86]. These care models reported positive outcomes on extending access to health services, enhancing affordability and improving effectiveness on disease or wellbeing indicators. The innovative aspect of social network models were the connections and relationships fostered between different actors and sectors [79, 84, 87]. Digital products such as mobile apps or online websites were leveraged to facilitate connections between actors. The outcomes of these models included positive behavioural change, building community social capital, and enhancing women’s participation and roles. The innovation within the entrepreneurial models were mechanisms to reduce costs of services [72, 82], while also improving access to services and creating new employment opportunities.
Followers
In the literature, creators of social innovation can operate either as individuals or as collectives, the latter including citizen movements, cross-disciplinary collaborative actor teams and institutions. The characteristics of individual social innovators in health are not well described, but three case studies offer insight into the role of personal experience, hardship or challenge, or of a community playing a significant contribution in the innovator’s work. Among the indigenous Maori population of New Zealand, innovations can often be constrained by culture and place, especially when diverted from acceptable mainstream western approaches [80]. However, social innovators in health used cultural, social and place-based capital to create solutions to serve their own communities [65, 80, 86]. In each case, community trust in the innovation was critical to its success.
The collective creation of social innovation in health (8/27 studies), either in cross-disciplinary actor teams or networks, has received greater attention. Firstly, the social innovation development process is used to overcome the siloed nature of health and to foster greater interdisciplinarity and intersectionality [61, 62, 66, 67, 69, 81, 82, 87]. This is particularly well illustrated in relation to Chagas disease in Guatemala, where innovation in interventions involved collaboration from epidemiology, biology, anthropology, sociology, engineering and architecture, and various funding agencies, international non-governmental organisations, government and universities [61]. The benefit of teams and collective networks is their capacity to move beyond boundaries and draw on collective cognition, capital, and the pooling and complementarity of capabilities [67].
Within these teams, opportunity was created for the participation of non-expert actors. As described in these articles [61, 74, 81], the value of social innovation from a public health policy perspective is the opportunity it affords less powerful actors (patients, families, beneficiaries, community members) to contribute to new health solutions, drawing on experiential knowledge and personal knowledge that can meaningfully contribute to and complement expert or academic knowledge. Applying social innovation as a process in itself leads to new forms of power relations and empowerment. The participation of actors in solution creation in some cases has translated into community action, but little beyond anecdotal evidence is presented in the health literature of sustained intervention success or actor empowerment [61, 73, 74]. Case studies from the management and development literature (3/27 studies) provide more depth and longitudinal evidence to substantiate the extent to which communities can be empowered, ensuring that self-governance and community autonomy of initiatives are achieved. The Kerala Palliative Care model, for example, has scaled far beyond its initial locus of implementation. From 1995 to 2012, 230 community organisations and 26 000 social activists became involved in the delivery of home-based services to 70 000 patients at the end of life [86]. The Graham Vikas social innovation in India also illustrates that the core to its approach is one hundred percent inclusion of members of the community, particularly women’s involvement in all decision-making processes. As a starting point, the program established a representative committee in each village, and a sustainability fund into which community members contributed, according to their means, to co-fund the work. Throughout project implementation, training was delivered on leadership, accounting and other operational procedures to ensure the community can fully manage the initiative independently [65]. Another example, the Business-in-a-Box initiative in Pakistan, illustrates how adopting a micro-entrepreneurship approach to extending access to contraception can empower women to become self-employed income generators while meeting their health needs [82].
In addition to embedding social innovations directly into communities, institutionalised actor networks can work to ensure sustainability. One model which has successfully embedded an initiative across multiple institutional levels is the Therapeutic Patient Education Model for Diabetes [77] in Austria. This case demonstrates the importance of social innovations engaging in institutional and political work with existing professional bodies at local and international levels, while creating new professional bodies to support its translation from research, its diffusion and its sustainability.
In summary, no category of actor is excluded from social innovation, irrespective of his/her background, organisational affiliation or hierarchical level. Across the literature, social innovation is seen as a democratising catalyst for health, enabling broad-based sectoral action, inclusion of marginalised individuals (including women) and providing communities with opportunities for action.
Values
To examine the principles and values upon which social innovations are based, articles were sub-classified according to the social innovation paradigm to which they ascribed. As illustrated above (Fig. 1), three main paradigms, nested within each other, exist: the instrumental or technocratic paradigm that accounts for social inclusion in the creation of new solutions; the democratic paradigm that accounts for the empowerment of actors through social innovation; and the institutional or structural paradigm that accounts for changes within existing institutions and systems. The majority of articles (16/27) upheld the instrumental or technocratic paradigm in which context social innovation was regarded as a solution to address challenges, and occurred through participatory processes that promoted the social inclusion of different actors. Although encouraging engagement in social innovation, this paradigm does not differ vastly from other approaches to public or patient participation and participatory governance in public health and development. These solutions offer improved ways to ensure greater effectiveness or efficiency, but do not transform relations or structures. These articles originate mainly from Europe, where the approach to social innovation has been influenced by the European Commission’s inclusion of the principle into policy with neoliberal agendas [45].
A second but smaller number of articles (8/27) engage with empowerment. These go beyond giving actors a voice or opportunity to provide input through consultation, and provide them with the opportunity to take control. By building the capacity of marginalised or under-represented actors, they develop an enhanced level of agency and action which suggests a change in power relations taking effect. Many larger-scale social innovation care models had people-centredness as a core organising principle [76, 80, 82]. Models were designed to involve not only the patient or the beneficiary at the health centre, but also health workers. The Buurtzog Neighbourhood Care model, for example, illustrated how, by enhancing patient and provider (nurse) autonomy, better outcomes in care provision were achieved and provider motivation and satisfaction were enhanced [76]. The iMOKO (New Zealand) and Business-in-a-Box (Pakistan) cases both illustrate empowerment of the local community by placing access to healthcare in the hands of trusted community members such as teachers, and by giving women in the community opportunities for income generation [80, 82]. The Time Bank model ascribed dignity and worth to the life of each person, and this highlighted the value of community members as active participants in healthcare: “The first core value of the Time Bank operations is asset, something of value to share with someone else … no one is worthless in the world … everyone is a contributor to society in his or her own way” [84]. Social innovations show how trusted community members such as teachers can play a vital role in promoting health and access to services; how women can play a role in the delivery of health products while being lifted from poverty through income generating opportunities; and how elderly people can be both consumers and providers of services [61, 62, 76, 80, 82, 84, 87].
The third and smallest number of articles (4/27) ascribed and recognised the systemic or structural paradigm of social innovation, and in the research, assessed the changes and dynamics that occurred at an institutional level. The research conducted by Vijay and Monin [86] in India adopted an institutional perspective to examine how certain contexts are more ‘poised’—receptive and ready—for social innovations. They also examined how actors, operating as institutional entrepreneurs, exercised agency to play an important role to increase the readiness of specific context to innovation and overcome the perceived resistance of existing institutions and structures. The Kerala Palliative Care model demonstrated large scale institutional change as it reframed palliative care provision from a medical frame to a social justice frame, with a professional hospice or hospital model replaced by the bottom-up organisation of services delivered primarily by community volunteers. The Therapeutic Patient Education Model for Diabetes revealed that, at the core of this initiative, systems level change was achieved by the institutional work of actors from national professional associations. They worked to embed the model into existing institutions (e.g. health insurance funds), while they created new institutions (new professional bodies) to ensure that new norms, values and practices were embedded at a systems level. Windrum et al. [77] recognised the potential of a model of patient centred care as having the potential of democratising medicine.
Lastly, research conducted by Pless and Appel [65] illustrated how social innovations can transform the norms, values, perceptions and roles within social institutions at community level through several approaches: the complete inclusion of all community members; the establishment of self-governing community structures; the provision of skills building; and service delivery. The project placed community members in the role of clients, so that project staff only acted upon community request. The long-term commitment (> 20 years) of this social innovation ensured that the outcome of an equitable and social society was achievable. This innovation recognised health as an outcome of sustainable development.
Facilitators and barriers
As a final part of the framework analysis, the facilitators and barriers of social innovations were considered that are relevant at different stages of the social innovation life cycle (Table 4). There were several commonalities across the literature in terms of enablers for idea development and implementation including: creating a safe, protective and facilitated environment; the democratic sharing of knowledge; the importance of timing and context; and implementing self-governance structures to support ongoing implementation and sustainability. Moving beyond the innovation locus to engage more broadly with partners and the existing system influenced innovation transfer, diffusion and scale. Only two studies—Therapeutic Patient Education Model and the Kerala Community Palliative Care model—described the process of institutionalising a social innovation [77, 86]. In both cases, a clear strategic approach was adopted by the innovators and implementers to replace prior institutional logics with new logics. This entailed deep contextual awareness and engagement in different forms of institutional work: advocacy to support movement building; locating the challenge in a moral or social justice frame; engaging existing institutions and creating new ones; and investing in the education of those involved in the innovation, both to attain legitimacy and ensure that standards can be maintained. Both of these social innovations have proven sustainable, and as models, they have been scaled to different settings and countries (Austria and India). Barriers negatively affecting across the various stages of social innovation development included cost considerations and resource constraints, a unreceptive or changing political context, limited evidence of effectiveness and implementer attitudes in terms of low motivation and drive.
